Low Back Pain & Pain Neuroscience Education (PNE): How to Integrate into Patient Care Without Scaring Patients Away
As you may know, the central nervous system and pain neuroscience has been very popular in the spine rehab industry over the last decade or so. And rightfully so! This was one of the main reasons I decided to do a neuro residency right out of PT school.
Since fear and uncertainty comes about A LOT when managing low back pain patients I figured I'd share with you what's been helpful for me as I started integrating pain neuroscience education with patients.
I feel very fortunate that one of my mentors during my neurological residency at Kaiser Permenente in Vallejo, CA was Stephen Schmidt PT, Mphysio, OCS, FAAOMPT. Stephen is a leader and international lecturer in pain neuroscience education one of the authors of “Integrating Manual Therapy and Pain Neuroscience”
If you’d prefer to listen👂🏽 instead of read content 👇🏽
CLICK HERE to tune into Episode 34 of The Spine PT Podcast 🎙️: “Pain Neuroscience & Back Pain: Breaking it Down for Patients”
My goal here is to share with you some of the actionable communication tools I learned from Stephen Schmidt and how I've integrated it into my practice with low back pain.
When you first realize that one of your clients REALLY needs to understand the fundamentals of pain science it can be overwhelming at first.
Certain clients are just very fixated on pain and for years they may have been told and truly believe that pain is an indication that they are still injured or that something is very wrong with their spine.
Guiding clients toward a paradigm shift in the way they think about pain, what it means, and how to utilize pain as information to take appropriate action can be a milestone in their recovery process.
A really effective way to start this paradigm shift is to first screen their knowledge about pain.
In the “Why you Hurt” index card curriculum by Adriaan Louw, there are about 12 pain knowledge true or false questions. For some, 12 questions can be overwhelming and time consuming so I’ve found it helpful to pick 2-3 questions that pertain best to each case to start.
Side note, Adriaan's short book for patients is also an AWESOME homework reading assignment to reinforce education we give in the clinic...
"Why Do I Hurt?"
Note: the images used in this article are from the "Why do I hurt" resources linked above
In my experience, I’ve found it useful to start the journey by screening the client’s understanding with these two questions:
1. When part of our body is injured, special pain receptors convey the pain messages to your brain: True/False
2. Nerves and their receptors adapt by increasing their resting level of excitement: True/False
Before continuing to read, answer these questions yourself first...
I'll answer these questions with a brief explanation and then explain them in a way I typically would with a client.
Something I learned very quickly from my mentor Stephen is that it’s REALLY important to immediately correlate this information with ACTIONABLE information and relate it back to their subjective history and our orthopedic assessment so that it is relatable to THEIR SPECIFIC situation.
So I'm trying to constantly relate this information back to their mechanical/neuro-orthopedic sensitivities:
Positional sensitivity
Load sensitivity
Neurodynamic Sensitivity (Slump test &/or PSLR)
Sensitivity to sustained postures
And how their specific sensitivities effect our plan of care decisions with respect to ergonomic adjustments like sleep/car/desk position, exercise selection, and manual therapy techniques.
So back to the true or false questions. Statement #1:
1. When part of our body is injured, special pain receptors convey the pain messages to your brain.
This statement is false. What we’ve learned is that there is actually no such thing as pain receptors in our body. Scientists once believed that there were pain receptors, so they performed studies where they took functional MRIs of someone's brain while they moved their painful low back.
A functional MRI allows us to see what part of the brain is the most active at any given moment (by means of oxygen uptake).
Neuroscientists thought if they could identify THE one area of the brain that was responsible for receiving pain messages, then they could surgically remove that area of the brain and all our pain problems would be solved.
But neuroscientists found out that there were several areas (8 or more) of the brain that were simultaneously active during a pain experience, and to make it more complicated the timing of activity in those areas changed moment to moment.
So what’s the deal?
Well, neuroscientists found out that instead of pain receptors, there are actually all different kinds of nerve receptors that are embedded all over our tissues that are responsible for alerting the central nervous system about a potential threat:
Chemical receptors: to detect inflammation in our tissues in the presence of an actual injury. Also, when an area of tissue doesn’t get blood/oxygen for a while the tissue becomes more acidic and that activates these receptors - aka ischemia/hypoxia
Temperature receptors: to detect temperature changes like when you touch something you weren’t expecting to be hot that is actually really hot.
Mechanical receptors: These are our movement receptors that detect changes in compression or tension within our tissues and joints.
Blood Flow receptors: to detect changes in blood flow since oxygen is the key for healthy tissues, its no surprise that our bodies have a built in redundancy between these receptors and chemical receptors (talk about a survival mechanism!)
Let’s talk about the 2nd true/false statement:
2. Nerves and their receptors adapt by increasing their resting level of excitement.True/False
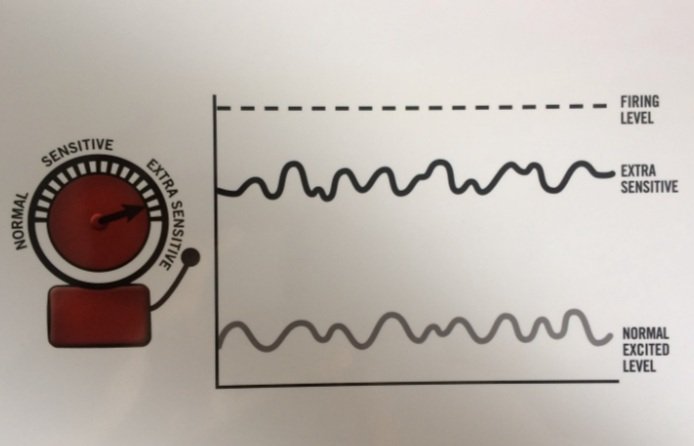
Image from “Why Do I Hurt?” booklet
This statement is true. All of our nerves have a resting level of electrical activity shown by the bottom wavy line in the photo above.
The dotted line at the very top represents something called an “Action Potential Threshold”.
Action potential threshold means that once the nerve’s receptors reaches this electrical threshold, the electrical impulse immediately shoots up to the higher order neurons to warn us that something is going on in our tissues (This is another protective mechanism for survival).
The diagram below is a great real life example of the action potential threshold, by thinking about what happens if we step on a nail.
Image from “Why Do I Hurt?” booklet
Whether it be an actual injury like stepping on a nail or a “repetitive stress” injury like too many reps of a poorly executed exercise OR sitting on the couch too long; if the chemical receptors or movement receptors’ (aka mechanoreceptors) activity reaches this threshold, a warning signal is immediately sent to the brain to get our attention to take appropriate action i.e focus and do the exercise with better form, attend to that wound from the nail, get off the damn couch or change position!
After an actual injury or with chronic pain the nerve’s resting level of activity remains elevated, hanging out close to the action potential threshold as a protective mechanism as shown below.
In the diagram above (Left image) represents the receptors' resting activity before the injury. The blue shaded area represents all the room you have for activity/movement before the receptors reach the threshold line and sends a warning signal to the brain.
As you can see in the image to the right, when the nerve’s resting level of activity hangs out close to the threshold line, there isn’t much room for activity/movement before the receptors’ activity reaches threshold and sends an impulse to the brain.
EXAMPLE OF PATIENT TALK TRACKS & NARRATIVES
Ok so that was the true/false answers & explanation... Here are some of the narratives that I'll try to weave into the discussion to make it practical with a patient case example... Imagine that you are now jumping into a conversation between a patient and I.
How can we use this information above to our benefit?
How can we help the tissue’s/nerve’s sensitivity come back down to baseline again so you can get back to your life?
By combining your subjective complaints along with our orthopedic exam, we will diagnose your specific low back pain using 4 Orthopedic Sensitivities.
Positional Sensitivity 2) Load Sensitivity 3) Sciatic Nerve Sensitivity (neurodynamic sensitivity) 4) Sustained Posture Sensitivity
The Orthopedic exam attempts to answer the following questions for us:
What positions are your joints and tissues sensitive to? These are the mechanical receptors in the your tissues telling us they are exhausted from this or that position!
Remember how forward bending re-created the low back pain but back bending didn't?
Are your tissues sensitive to Load, compression, weight bearing, the influence of gravity? Basically, are the symptoms a little better when we manually decompress your joints & tissues or when you simply just lay down and take a load off? Again these are the mechanical receptors in the tissues trying to tell us they are exhausted from being compressed all the flipping time.
Remember how rounding your back in standing & sitting hurt, but it didn't hurt to round your back on all fours or laying on your back?
Are your nerves sensitive when we yank on them and tension (neural tension) them? Again these are the mechanical receptors in the sciatic nerve that tell us that the nerve keeps getting pulled on all day long by sitting the way you do or by stretching your hamstrings the wrong way.
Nerves are blood thirsty animals and they are not as elastic as our muscles, tendons, and ligaments. They are designed more like brake cables and when you pull on them they actually don’t stretch that well. The tension actually shunts away blood and now the nerve is getting less blood and oxygen while being pulled on. Yeah, this will keep your nerves extra sensitive for sure, nerves hate this kind of environment!
Is your body sensitive to sustained postures? Or lack of movement? Like sitting too long and not being active (forget the word “exercise”, we’re talking about movement). This message is the chemical and blood flow receptors talking to us. No movement = less blood = less oxygen = more acidic environment in the tissues. Now add this to a situation where you’re in your positional sensitivity, a little bit of load, and sprinkle on some sciatic nerve tension and you have a perfect receipt for chronic hypersensitivity of your tissues aka Chronic sciatica & low back pain.
The combination of these variables gives us your “Functional Low Back Pain Diagnosis”.
For example your low back seems to be sensitive to the rounded position (flexion) because when you back bend or arch your back you said it doesn't feel as bad.
When we have you sit, round your back, straighten your knee, and bend your ankle at the same time, we’re actually stretching you sciatic nerve and your body told us it definitely didn’t like that (I'll use the image below as reference while educating).
You also told me that driving was the worst. Your Functional diagnosis is Flexion sensitive low back pain that is complicated by load sensitivity and sciatic nerve tension on that right side.
We’re going to use that information to adjust your car seat and the way you sit at work to minimize your low back's exposure to that sensitive rounded position while we stop yanking on your sciatic nerve to desensitize your back & your nerve.
We’re going to teach you how to decompress your own spine through different self -traction techniques that you can do throughout the day. This is helping you manage the load sensitive component.
This will also help improve circulation throughout the tissues in you back.
For example, the discs in our spines don’t get the greatest circulation compared to muscles because discs’ tissues are more built like a combination of ligaments and cartilage.
So when we decompress the spine this allows for the discs to breathe a little bit aka get some blood & oxygen. This will also help desensitize the tissues in your back so that you have less pain and are more free to move.
We will also start some manual therapy and exercise to promote low level movement through your low back to help improve blood flow, circulation, and flush out any left over inflammation, if there is any.
Giving tissues blood/oxygen has been shown to reduce sciatic nerve sensitivity. This is why figuring out some type of low level cardiovascular activity for you to do.
This doesn't mean you need to do hours of cardio. The good news is that the minimum effective dose to reduce nerve sensitivity has been found to be 10 minutes of keeping your resting heart rate above 20 beats per min. So yes, just 10 minutes of continuous walking is doing something.
This minimal effective dose of cardio also taps into the most potent "internal pain medication" we have available to us. They are chemicals in the brain that have found to be released with low-level cardio like enkephalins, serotonin, & endorphins.
The medications that are made by pharmaceutical companies and prescribed by doctors attempt to imitate these neurochemicals released in our brain when we do cardio.
Getting back to movement and exercise can be really tricky so it’s important that we treat movement/exercise just like we would medication. Two advils will help reduce your headache, but 6 advils will give you undesirable side effects. Exercise is no different!
If you walk for 30 min and then you start to feel the pain, don’t freak out! This information is gold!
This doesn’t mean you re-injured yourself. You just found your back's threshold that we need to learn how to flirt with.
We need to listen to your body’s sensitivity and adjust our plan. Respect this threshold but don’t be scared of it. Flirt with it. If 30 minutes triggered pain >6/10 then next time we walk for 25 min and see how it feels over 24-48hrs. We can then add 1 minute each time after that. This is what we call "slow cooking" your activity tolerance.
Remember that most of us expect progress to look like the red image below, where as in reality progress looks more like the green image. Try not to fixate and getting attached to what you think your body "should be able to do", check the ego at the door, find your current level of ability and we'll adjust our approach accordingly.
I hope this article helped you envision what blending low back pain & pain neuroscience education can look like to help manage the fear of uncertainty that frequently comes up when managing these patients.